A palliative care nurse has opened up to Breaking News Today about her daily struggles during the coronavirus pandemic, saying her job is “really, really hard” at the moment.
Jenna Norris, who works at the Shakespeare Hospice in Stratford-upon-Avon, revealed that her team of nurses are “coping well” but that they are struggling with the ban on physical contact and the fact that they have to wear a protective mask and visor when they see their patients.

She said: “We’re normally very tactile with our patients and their families. We use touch a lot as a method of comfort… giving someone a hug or holding their hand. Not being able to do that at the moment is really, really hard. Also our job involves a lot of difficult conversations and having to have those conversations through a mask or a visor is really tough and just feels unnatural.”
She added: “It feels like it’s a barrier between our communication that we’re not used to, and it feels really impersonal.”
Take a look at the Coronavirus stats in the UK, live right now!
Jenna offers medical and emotional support to her patients in the local area, making twice-daily visits.
She revealed that the demand for her services has gone up in recent weeks since the coronavirus pandemic arose. However, her NHS colleagues in the community were supporting her to ensure that everyone who is requiring end of life care at their home gets what they need.
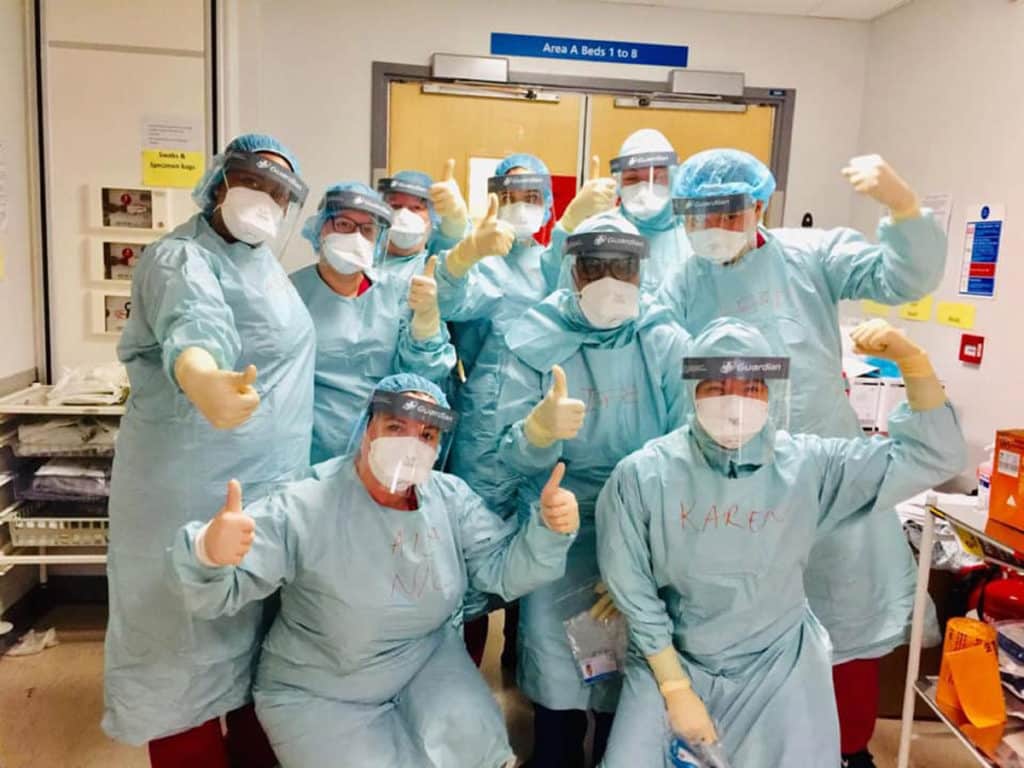
She said: “We’re very good at supporting each other and reflecting on things, and that’s needed even more at the moment.”
Currently, NHS England guidelines state that families will be expected to provide end of life care to relatives dying at home during the COVID-19 crisis.
It says: “During the coronavirus pandemic, there will be more people dying of coronavirus at home who will require care and support at the end of their lives. The anticipated increase in demand and stretch in workforce availability means that there will have to be a greater reliance on family members, unpaid carers and those who are with these patients to help provide care.”
It adds: “They may have to administer medication more than they are used to.”
Caroline Abrahams of Age UK expressed her concern that this could lead to patients being left unsupported and even at risk.

She said: “The guidance talks about delivering palliative care remotely, but how is that possible? In a valiant and right attempt to protect the NHS staff from contracting the virus, people are being left on their own when they need support.”
She went on to say: “Where are the safeguarding measures to stop people being bumped off? Helping someone die well is a specialist skillset. Unfortunately, it feels as though people have been left to get on with it when a reasonable expectation of our society is that we get skilled palliative care.”

Prof Martin Marshall, the chair of the Royal College of GP’s, said: “COVID-19 is more than an NHS issue – it will take a nationwide effort to get through this crisis and so far, we have seen a tremendous effort from our patient’s families and friends. Where families are not comfortable taking on elements of their loved one’s care, this will be respected.”
